Women's Health
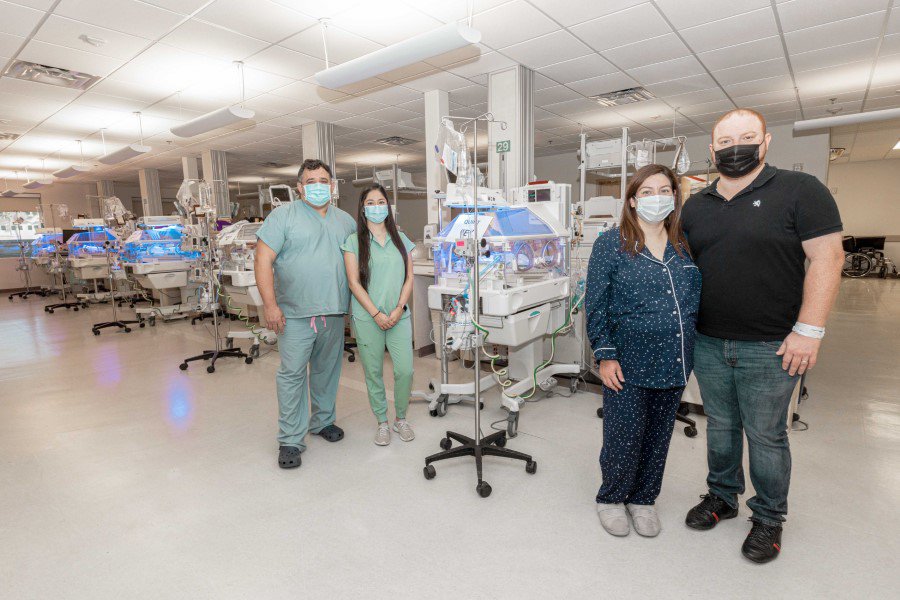
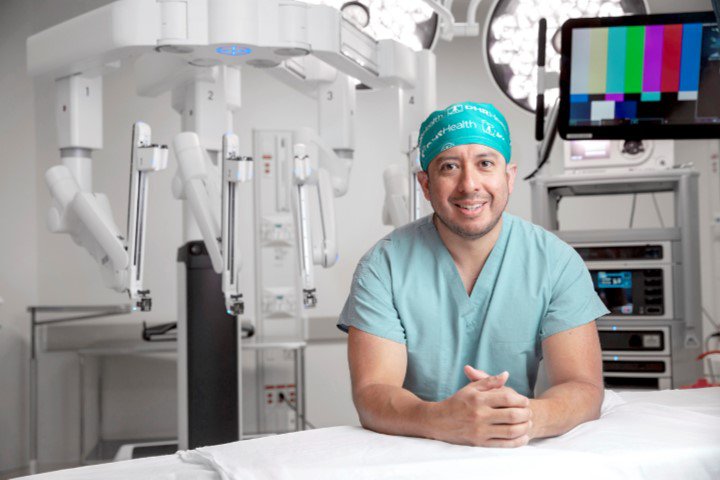
At DHR Health Women’s Hospital, we are proud to be the first and only designated Level IV Maternal Facility in the Rio Grande Valley, recognized by the Texas Department of State Health Services for providing the highest level of comprehensive maternal care. This prestigious Level IV designation reflects our capability to manage the most complex maternal cases. Our services include comprehensive care for non-complicated to high-risk pregnancies, advanced gynecology, and innovative robotic surgery, ensuring that every aspect of women’s health is covered with exceptional, dedicated care. Our team of specialists is committed to delivering the highest standard of treatment and support to every patient.
Helpful Links